Robotics technology brings better health services to remote communities
- Andréa Ledding | October 01, 2016
The University of Saskatchewan College of Medicine has partnered with the government of Saskatchewan to bring cutting-edge remote technology to better serve northern Indigenous communities.
“One of the issues is if you’re in Pelican Narrows and you have an emergency situation — a kid that has a respiratory tract infection — you go to the nursing station,” explained Dr. Ivar Mendez. But the problem is there are no doctors present, and patients in distress need to be driven or flown to the nearest doctor or hospital, which takes at least a few hours: potentially lethal for the child. “We actually bypass that, we bring the specialist in real-time at the time the patient needs it.”
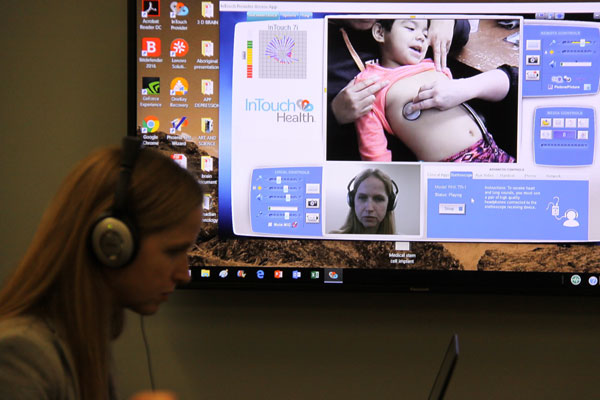
A robot allows the doctor to assess the patient using remote access technology with the assistance of the nursing station. This also builds capacity for the nurses, and the patients and their family, explained Mendez.
Attachments allow eye, ear, mouth, lungs, skin, and ultrasound/laboratory examination. Mendez noted that northern First Nations communities are particularly underserved in terms of prenatal care and pediatric care, which has a high impact on infant and neonatal mortality. Robotic access addresses this, while patients are provided services in their communities.
“We’re able to send expertise that’s accessed in real time,” explained Mendez. Pediatric specialist Dr. Tanya Holt then examined a four-year-old in Pelican Narrows via the remote robot, prescribing medication and protocol changes.
Holt explained that prior to the robotic technology, travel by vehicle or flight was necessary to see a specialist. Now they can connect within seconds or minutes and perform life-saving supportive diagnostics and therapy immediately.
“There’s a lot of evidence that initiating care early and in a timely fashion improves outcomes in the pediatrics and adult population, and if we can improve the timeliness of our care, we may actually see better outcomes across the board,” noted Holt. She said Saskatchewan’s geography makes it difficult for quick access to tertiary care, saying that quick response time saves lives. “With every hour that passes without therapy there’s a twofold increase of mortality.”
Remote presence technology has the potential to save lives, while being more convenient, allowing patients and their families to mostly remain within their communities. Mendez noted that the community was the leader in pointing out the need, saying pediatric care was a priority, and the pilot has gone better than their expectation.
“60% were able to be treated without being transported, and of the 40% they were able to be regionalized,” said Mendez. Additionally the rotation and recruitment of nurses has improved because they have the support to care for patients. “The 24 children that didn’t have to be transported saved $240 000...but [savings was ] also in terms of the lives of these young families that didn’t have to come to Saskatoon.”
They plan to recreate the success of Pelican Narrows in other communities with their remote presence medicine, saying it is like the internet or cellphone technology.
“The rest of the world adapts to technologies that make sense,” said Mendez. “We are really pushing boundaries, we are pioneers in the country. There is no other centre in Canada that has a remote presence technology...we are pioneers on an international level.”
He also noted that it allows for care in a culturally appropriate manner, which Dr. Veronica McKinney explained, empowering local people with medical knowledge.
“Greater than 85% are Indigenous...about 40 000 people in 70 communities, in an area just a little smaller than the Yukon,” noted McKinney. “This allows people to get the care right where they are...it supports the families.”
They will be working with communities, health regions, and bands, to implement more locations.