
Eczema the diabetes of dermatology
Canada’s first Indigenous dermatologist, Dr. Rachel Asiniwasis, is looking to understand why so many Indigenous people have uncontrolled eczema.
“Is it because, genetically, Indigenous people are more prone to skin disease? Unfortunately, that’s something that there’s no information on,” said the dermatologist who is also a member of Muscowpetung Saulteaux Nation. “I would argue, that in my experience, the conditions seem strikingly more severe, especially in remote communities where there are more barriers to receiving care.”
Atopic dermatitis, or eczema, is a well-known skin condition, but Asiniwasis said, it’s actually far more serious than most people realize.
Eczema is a condition that causes dry, itchy, and inflamed skin. It is most common in young children but can occur at any age and is chronic with regular flares.
“I call eczema the ‘diabetes of dermatology’, because its the most common chronic skin condition that is inflammatory,” she said. “There’s lots of misconceptions that it’s just a skin problem. But because of the skin barrier being impaired, patients with eczema are unable to hold water and moisture in their skin and are prone to developing infections.”
The side affects of eczema can run much deeper.
Patients sometimes experience constant itchy skin that can bleed and disturb sleep. The condition can lead to depression and anxiety, as well as decreased performance at work and school, explained Asiniwasis.
In addition, eczema is linked to the development of asthma and allergies down the road, she said.
Research shows that eczema can also affect the inside of the body and may even affect bone health or even cause cardiovascular disease.
“You can imagine, it can really influence people in their career choices, it’s a really impactful disease,” said Asiniwasis. “If you ignore eczema and children get infected, their skin can thicken, and they can end up with mental health issues.”
About 90 per cent of those with eczema develop conditions before the age of five.
Data is limited for specific impacts on Indigenous communities, but Asiniwasis said the national average for Indigenous youth is about 10 per cent. But she’s seeing around 16 per cent in Saskatchewan communities, with eczema affecting as much as 25 per cent of youth in northern and remote communities.
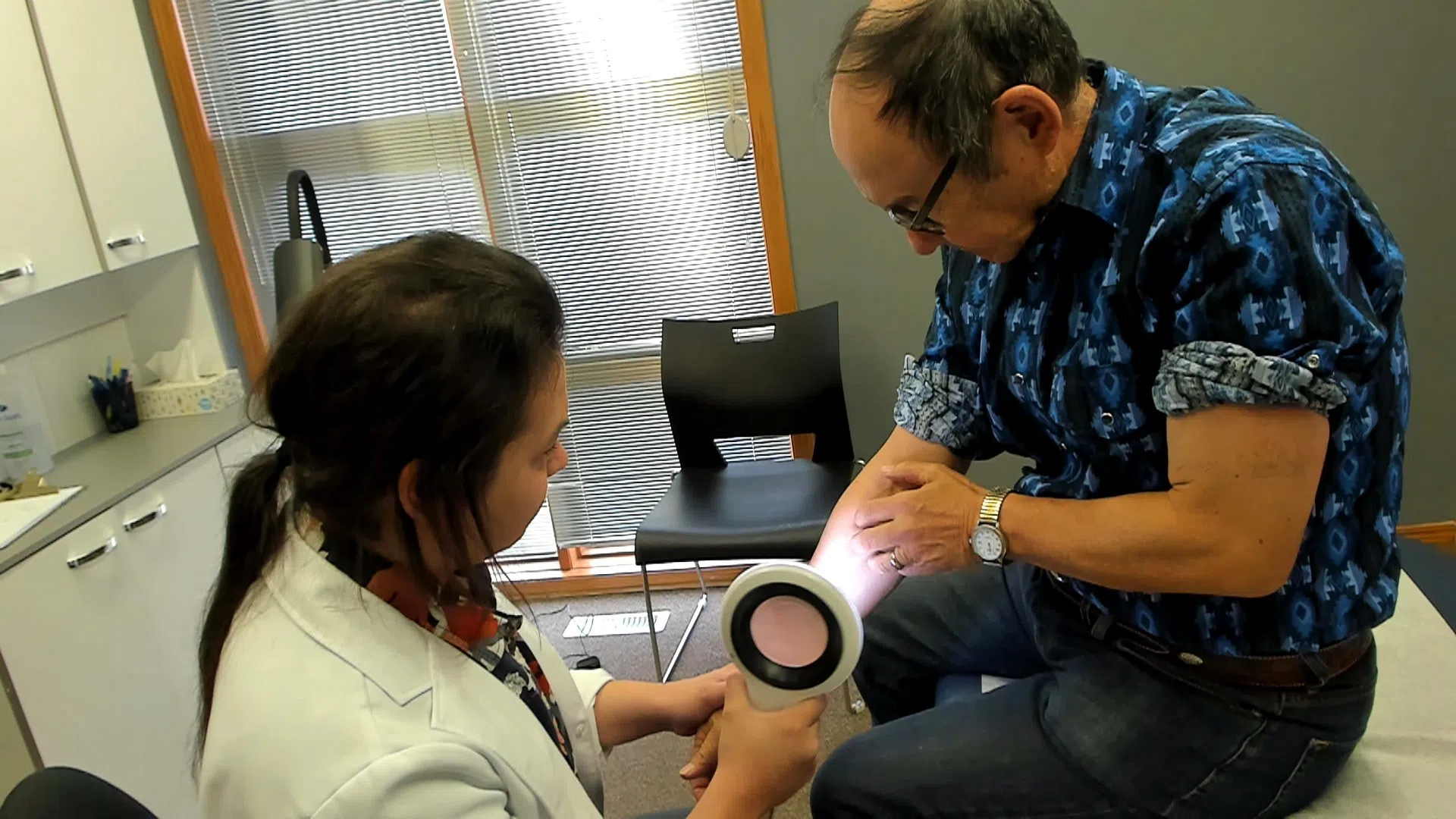
Photo by Ashley Emmens
Jennifer McGillis, a Métis and First Nations woman from Regina, has dealt with eczema for most of her life, starting when she was around eight years old.
“I used to have it on the back of my legs and arms, so when I would wear shorts, I would get bullied because they didn’t know what it was,” she said.
McGillis still suffers from the condition, with itchy patches on the top of her hands. She said her children and grandchildren also have eczema, including two-year-old grandchildren who have itchy breakouts, cannot use many kinds of soap or detergent, and sometimes cannot wear diapers or clothes entirely.
She said none of the treatment she’s received from family physicians has been ineffective.
“I’ve always been told to go to a dermatologist because the doctor didn’t know (how to treat the case),” said McGillis. “I have three different types of cream from the doctor, none of which really work.”
So, what needs to change to address this issue affecting so many young Indigenous people?
Asiniwasis said it starts with engaging Indigenous communities and empowering them in these kinds of projects, as there is a lack of representation of Indigenous people in these studies.
“We’re missing information on the experiences and values of Indigenous patients. We need to have hear their stories and expand beyond just numbers,” she said. “We need to learn about the barriers and determinants of health and talk about solutions.”
The barriers to treating eczema are vast such as: A lack of access to healthcare for patients in remote communities; Overwhelming instructions on how to care for the condition; Both frontline workers and patients downplaying the condition; as well as language issues.
“I hear very often from my patients that ‘my family doctor didn’t have time to talk about my skin condition, (the doctor) didn’t know what to do, or dismissed it outright’,” said Asiniwasis.
Indigenous leaders, healthcare workers, patients, and researchers need to engage with each other, said Asiniwasis, to develop strategies to address this issue.
“We need to engage communities and document it as best we can. I think we all need to come together and look at this closer,” she said. “That way, policy makers have to address it.”

